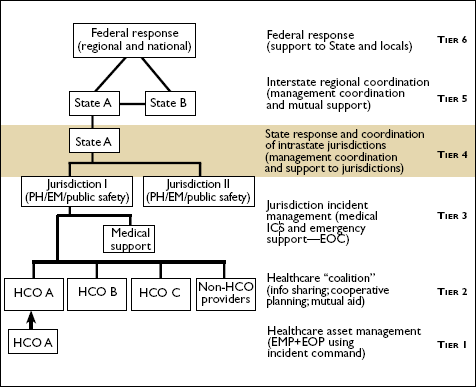
Tier 6 consists of Federal public health and medical assets (e.g., supplies, equipment, facilities, and personnel) organized under Emergency Support Function (ESF) #8 of the National Response Plan (NRP). The U.S. Department of Health and Human Services (HHS) is the Primary Agency for ESF #8 and coordinates Federal public health and medical assistance in support of State, Tribal, and jurisdictional response efforts.[70]
Key Points of the Chapter
The Federal Government may provide public health and medical assistance during an emergency or disaster under ESF #8 of the NRP. This assistance can be activated by a Presidential declaration of a major disaster or emergency, declaration of an Incident of National Significance by the Secretary of the Department of Homeland Security (DHS), or at the request of another Federal department or agency. HHS can also provide public health and medical assistance during an emergency or disaster under the independent authority of the Secretary of HHS.
The primary role of Federal resources in providing medical surge capacity and capability (MSCC) is to support, not supplant, State, Tribal, and jurisdictional response efforts. When the NRP is triggered by a Presidential declaration of a major disaster or emergency under the Stafford Act, Federal assistance generally is provided at the request of the Governor (or his/her designee) of an affected State. In a catastrophic event,[71] however, Federal assets may be mobilized and deployed to Federal installations in advance of a formal request for assistance. The Catastrophic Incident Supplement of the NRP establishes the policies, procedures, and mechanisms by which this may occur. The Federal Government closely coordinates this proactive mobilization with affected States, Tribal Nations, and jurisdictions.
On behalf of the Secretary of HHS, the Assistant Secretary for Preparedness and Response (ASPR) coordinates all aspects of Federal public health and medical assistance under ESF #8. The HHS Secretary's Operations Center (SOC) is the hub of information management and strategic-level command and control for ESF #8. During an emergency, the HHS Emergency Management Group (EMG) operates out of the SOC to coordinate the ESF #8 response. The ASPR may request that liaisons from the ESF #8 support agencies[72] and HHS Operating Divisions (OPDIVs)[73] be provided to the SOC to ensure a coordinated ESF #8 response. () Similarly, HHS may provide liaisons to other Federal, State, Tribal, and jurisdictional Emergency Operations Centers (EOCs) to promote response coordination. The SOC also provides liaisons to appropriate Federal command and control posts identified in the NRP, such as the National Response Coordination Center or the National Operations Center.
The HHS Incident Response Coordination Team (IRCT), which is mobilized by the ASPR, coordinates all deployed ESF #8 assets. All field communications to the SOC flow through the IRCT, which is typically led by an HHS Regional Emergency Coordinator. The IRCT team leader is accountable for executing field activities for the ASPR. In a large-scale or complex incident, the Secretary of HHS may also deploy a Senior Health Official (SHO) to be his/her direct representative in the field. When deployed, the SHO is responsible for overarching coordination of deployed ESF #8 assets and provides guidance and leadership to the IRCT. The SHO serves as the senior-level ESF #8 liaison to State, Tribal, jurisdictional, and other Federal officials, including the DHS-appointed Principal Federal Official. The SHO operates at the strategic level and reports to the EMG. Typically, the SHO is part of the PFO Coordination Cell and coordinates with the IRCT leadership.
To promote an effective ESF #8 response, preparedness activities should examine and clearly delineate the processes for requesting, receiving, and managing Federal assistance. State, Tribal, and jurisdictional public health and medical planners must precisely determine their response capability, when they might need Federal support, how to develop and submit a request, and how they would integrate Federal assets into their incident command system.
7.1 The Role of the Federal Government in MSCC
Should incident needs severely challenge or exceed State, Tribal, and jurisdictional response capabilities, Federal resources may be called on to provide additional surge capacity and capability. When this occurs, Federal agencies and resources function in support of State, Tribal, and jurisdictional response efforts. When catastrophic events overwhelm State, Tribal, and jurisdictional response capabilities, Federal resources can be mobilized in advance of a formal request for assistance per the Catastrophic Incident Annex of the NRP; however, the proactive deployment of these resources is closely coordinated with affected State, Tribal, or local authorities.
The authority for Federal public health and medical response may come from a Presidential declaration of a major disaster or emergency (commonly known as a Stafford Act declaration), a declaration of an Incident of National Significance by the DHS Secretary, at the request of another Federal department or agency, or under the Public Health Service Act.
Robert T. Stafford Disaster Relief and Emergency Assistance Act: At the request of the Governor of an affected State, the President may declare a major disaster or emergency if an event is beyond the combined response capabilities of the State, Tribal, and jurisdictional governments. Among other things, this declaration allows Federal assistance to be mobilized and directed in support of State, Tribal, and jurisdictional response efforts. Under the Stafford Act, the President can also declare an emergency without a Gubernatorial request if primary responsibility for response rests with the Federal Government because the emergency involves a subject area for which the United States exercises exclusive responsibility and authority.
Incident of National Significance: The DHS Secretary, in consultation with other Federal departments and agencies, and the White House, as appropriate, may declare an Incident of National Significance.[74] With this declaration, the Secretary of DHS implements any or all of the applicable coordinating structures and processes described within the NRP, as required by the incident.
Public Health Service Act: The Secretary of HHS has the independent authority under section 319 of the Public Health Service (PHS) Act, as amended, to declare a public health emergency. Following a section 319 declaration, the Secretary can, among other things, take appropriate actions in response to the emergency, such as conducting and supporting investigations into the cause, treatment, or prevention of the disease or disorder. The Secretary can also waive certain Medicare and Medicaid requirements to ensure sufficient health care items and resources are available to individuals enrolled in Social Security Act programs. The Secretary may use his/her discretion in determining whether an event is of sufficient severity or magnitude to warrant such a declaration. The Secretary has other authorities under the PHS Act that can be exercised independent of a declaration. The Secretary can make and enforce regulations to prevent the introduction, transmission, or spread of communicable diseases into the U.S., or from one State or possession to another; deploy personnel from the U.S. Public Health Service (USPHS) Commissioned Corps in support of public health and medical operations; provide public health and medical services; and provide for the licensure of biological products.
Federal public health and medical assistance consists of medical materiel, personnel, and technical assistance. These resources may provide response capability for the triage, treatment, and transportation of victims or persons with special medical needs; evacuation of patients; infection control; mental health screening and counseling; environmental health services; and other emergency response needs. Below is an example of the full range of support available through ESF #8. A variety of Federal public health and medical assets may be provided, including the following:
USPHS Commissioned Corps
National Disaster Medical System (NDMS)
Strategic National Stockpile (SNS)
Federal Medical Stations (FMSs)
Assets from the Department of Veterans Affairs (VA), the Department of Defense (DoD), and other Federal assets.
Medical Reserve Corps
ESF #8 involves supplemental assistance to State, Tribal, and jurisdictional governments in identifying and meeting the public health and medical needs of victims of major disasters or public health emergencies. This support is categorized in the following functional areas:
Assessment of public health/medical needs
Public health surveillance
Medical care personnel
Medical equipment and supplies
Patient movement
Hospital care
Outpatient services
Victim decontamination
Safety and security of human drugs, biologics, medical devices, veterinary drugs, etc.
Blood products and services
Food safety and security
Agriculture feed safety and security
Worker health and safety
All hazard consultation and technical assistance and support
Mental health and substance abuse care
Public health and medical information
Vector control
Potable water/wastewater and solid waste disposal, and other environmental health issues
Victim identification/mortuary services
Veterinary services.
In addition, the Federal Government may temporarily waive or modify certain normal requirements of Federal programs during a national emergency or disaster that is also a public health emergency to facilitate the delivery of public health and medical assistance. For example, Section 1135 of the Social Security Act authorizes the Secretary of HHS to temporarily waive or modify normal operating requirements of Medicare, Medicaid, or the State Children's Health Insurance Program (SCHIP) during a national emergency or disaster declared by the President that is also a public health emergency declared by the HHS Secretary (see below). This action ensures that affected healthcare providers who are unable to comply with certain Federal requirements because of a national emergency or disaster that is also a public health emergency, but who operate in good faith, are given sufficient flexibilities to continue providing services to beneficiaries and receive reimbursement for those services.
Waiving Healthcare Requirements in Hurricane Katrina
One way the Federal Government facilitates the delivery of medical care and public health services during a major emergency or disaster is by temporarily waiving or modifying normal operating requirements of Federal programs. For example, during the response to Hurricane Katrina, the Secretary of HHS, pursuant to Section 1135 of the Social Security Act, waived the following requirements:
Certain conditions of participation, certification requirements, program participation or similar requirements, or pre-approval requirements for individual healthcare providers or types of healthcare providers, including, as applicable, a hospital or other provider of services, a physician or other healthcare practitioner or professional, a healthcare facility, or a supplier of healthcare items or services
The requirement that physicians and other healthcare professionals hold licenses in the State in which they provide services, if they have a license from another State (and are not affirmatively barred from practice in that State or any State in the emergency area)
Sanctions under Section 1867 of the Act (the Emergency Medical Treatment and Labor Act, or EMTALA) for the redirection of an individual to another location to receive a medical screening examination pursuant to a state emergency preparedness plan or transfer of an individual who has not been stabilized if the redirection or transfer arises out of hurricane-related emergency circumstances
Limitations on payments under Section 1851(i) of the Act to permit Medicare Advantage enrollees to use out-of-network providers in an emergency situation
Sanctions and penalties arising from noncompliance with the following provisions of the HIPAA privacy regulations:
The requirements to obtain a patient's agreement to speak with family members or friends or to honor a patient's request to opt out of the facility directory
The requirement to distribute a notice of privacy practices
The patient's right to request privacy restrictions or confidential communications.
The 1135 waiver typically ends with the termination of the emergency period, or 60 days from the date the waiver is first published unless the Secretary of HHS extends the waiver by notice for additional periods of up to 60 days. During Katrina, waivers for EMTALA and HIPAA requirements were in effect for a period not to exceed 72 hours from implementation of a hospital disaster protocol. The 1135 waiver applies only to Federal requirements and does not automatically apply to State requirements for licensure or conditions of participation.
7.2 Federal Emergency Operations Plan
As required by Homeland Security Presidential Directive (HSPD)-5, the NRP establishes the structure and process for systematic, coordinated, and effective delivery of Federal assistance to augment State, Tribal, and jurisdictional response capabilities.[75] It describes Federal resources that are available to mitigate, prepare for, respond to, and recover from major emergencies and disasters. In addition, the NRP outlines the mechanisms for mobilizing and integrating Federal support. While the NRP is always in effect, its implementation is scalable and flexible to meet the unique operational and information sharing requirements of any major threat, disaster, and emergency, including acts of terrorism.
The types of direct Federal assistance that States, Tribal Nations, and jurisdictions may need, as well as the operations support required to sustain Federal response (e.g., transportation, communications), are organized in the NRP under ESF annexes. Each ESF is coordinated by a Primary Agency designated on the basis of its authorities, resources, and capabilities in a particular functional area. Federal public health and medical assistance is provided under ESF #8, and HHS serves as the Primary Agency to coordinate ESF #8 resources to fulfill the requirements identified by the affected State(s), Tribe(s), and jurisdictional authorities. HHS may also support other ESFs, most notably ESF #6—Mass Care, Housing, and Human Services.
Pursuant to HSPD-5, the Secretary of DHS is responsible for the overall coordination of Federal resources under the NRP. During an event, the Secretary of DHS may designate a PFO to act as his/her representative in the field to oversee, coordinate, and execute Federal incident planning and response activities. The Secretary also relies on a host of multiagency coordinating structures at the Federal headquarters, regional, and field levels. These structures, some of which were recently modified in the May 2006 update of the NRP, include the following:[76]
National Operations Center (NOC): The NOC replaces the Homeland Security Operations Center (HSOC) as the central point for Federal incident management, interagency coordination, and information sharing. One of the key functional elements of the NOC is the National Response Coordination Center (NRCC), which coordinates the overall Federal response and recovery for Incidents of National Significance and emergency management program implementation.[77]
Incident Management Planning Team (IMPT): The IMPT provides contingency and crisis incident management planning in support of DHS national domestic incident mission requirements. It is composed of a core group of full-time senior planners who are assigned to the IMPT from interagency and DHS offices for a period of one year. In addition, there is pre-identified on-call staff to augment the IMPT core staff when required.
Domestic Readiness Group (DRG): The White House convenes the DRG on a regular basis to develop and coordinate implementation of preparedness and response policy. The DRG is also convened in anticipation of or during crises such as natural disasters and domestic terrorists attacks to address issues that cannot be resolved at lower levels, and to provide strategic policy direction for the Federal response.
Regional Response Coordination Center (RRCC): Within each of its regions, the DHS/Federal Emergency Management Agency (FEMA) may establish an RRCC to coordinate regional response efforts, establish Federal priorities, and implement local Federal program support until a Joint Field Office is established. The RRCC communicates with the affected State Emergency Operations Center (State EOC) and the NRCC, deploys teams to conduct initial damage assessments, and issues initial mission assignments.
Joint Field Office (JFO): The JFO is a temporary Federal facility established locally where Federal, State, Tribal, and local executives with responsibility for incident management coordinate, oversee, and direct prevention, preparedness, response, and recovery activities. It is organized according to the principles of the National Incident Management System (NIMS) around a JFO Coordination Group, as well as Operations, Planning, Logistics, and Administration/Finance Sections. The JFO Coordination Group may include a Principal Federal Official (PFO), designated by the DHS Secretary to be his/her representative locally to coordinate overall Federal incident management and assistance activities.
In the event of multiple incidents, or one incident with widespread implications (e.g., Hurricane Katrina), multiple JFOs may be established at the discretion of the Secretary of DHS.
The NRP is built upon the NIMS, which provides the core doctrine, terminology, and organizational processes for coordinated multidisciplinary and intergovernmental incident management. This includes uniform personnel qualifications and standards for equipment and communications. These concepts are necessary for interoperability and compatibility. The NIMS management framework is applicable to all hazards regardless of cause, size, or complexity. The Incident Command System (ICS) is put forth by NIMS as the model for organizing and managing emergency personnel and resources during incident response.[78] The NIMS requires that field command and management functions be performed in accordance with standard ICS organizations, doctrine, and procedures.
7.3 Emergency Support Function #8
When incident needs challenge or exceed the medical or public health response capabilities of local, State, Tribal, or regional response assets, Federal public health and medical assistance may be made available under ESF #8 of the NRP. This support may be provided in response to a variety of public health and medical events, including the following:
Natural and man-made disasters and public health and medical emergencies
Terrorist threats or incidents using chemical, biological, nuclear/radiological, or large explosive devices
Infectious disease outbreaks and pandemics
Animal health emergencies, such as those in support of ESF #11 (e.g., Bovine Spongiform Encephalopathy, Hoof and Mouth Disease)
Any other circumstance that creates an actual or potential public health or medical emergency where Federal assistance may be necessary.
The Pandemic and All Hazards Preparedness Act amended section 2801 of the PHS Act to state that the Secretary of HHS shall lead all Federal public health and medical response to public health emergencies and incidents covered by the NRP. Federal public health and medical assistance provided under ESF #8 of the NRP may be categorized according to the functional areas described below.
Assessment of Public Health/Medical Needs: HHS, at the request of DHS, mobilizes and deploys ESF #8 personnel to support the Emergency Response Team-Advance (ERT-A)[79] to assess public health and medical needs. This function includes the assessment of the public healthcare system/facility infrastructure.
Health Surveillance: HHS coordinates with State, Tribal, and jurisdictional officials to do the following:
Establish surveillance systems to monitor the health of the general population and special high-risk populations
Conduct field studies and investigations
Monitor injury and disease patterns and potential disease outbreaks
Provide technical assistance and consultations on disease and injury prevention and precautions.
Medical Care Personnel:
Medical response capabilities are provided by assets internal to HHS (e.g., USPHS Commissioned Corps, the National Disaster Medical System (NDMS)).
DoD may be requested to provide support in casualty clearing/ staging and other missions as needed.
HHS may seek individual clinical health and medical care specialists from the VA to assist State, Tribal, and local personnel.
Health/Medical Equipment and Supplies: HHS may request that agencies provide medical equipment and supplies, including Federal Medical Stations (FMSs) that provide low acuity medical care, pharmaceuticals, and biologic products (e.g., SNS), etc., in support of immediate medical response operations and for restocking healthcare facilities in an area.
Patient Evacuation:
HHS may request that DHS/FEMA and ESF #1 provide support to DoD for patient movement in the evacuation of seriously ill or injured patients from the affected area to locations where hospital care or outpatient services are available.
DoD is responsible for regulating and tracking these patients to appropriate treatment facilities (e.g., NDMS non-Federal hospitals, VA hospitals, and DoD military treatment facilities).
Patient Care: HHS may request available personnel to support in-hospital care and outpatient services for victims who become ill or injured.
Safety and Security of Human Drugs, Biologics, Medical Devices, and Veterinary Drugs, etc.: HHS ensures the safety, efficacy, and security of regulated foods, human and veterinary drugs, biologics (including blood and vaccines), medical devices (including radiation emitting and screening devices), and other HHS regulated products.
Food Safety and Security: HHS, in cooperation with ESF #11, ensures the safety and security of Federally regulated foods.
Blood and Blood Products: HHS establishes and maintains contact with the American Association of Blood Banks Inter-organizational Task Force on Domestic Disasters and Acts of Terrorism[80] and, as necessary, its individual members, to determine:
The need for blood, blood products, and the supplies used in their manufacture, testing, and storage
The ability of existing supply chain resources to meet these needs
Any emergency measures needed to augment or replenish existing supplies.
Agriculture Safety and Security: HHS, in coordination with ESF #11, ensures the safety and security of animal feed and therapeutics.
Worker Health/Safety:
HHS requests Department of Labor (DOL) assistance to coordinate responder and worker safety and health using processes detailed in the Worker Safety and Health Support Annex.
HHS requests support, as needed, to assist in monitoring the health and well-being of emergency workers; performing field investigations and studies addressing worker health and safety issues; and providing technical assistance and consultation on worker health and safety measures and precautions.
All-Hazard Consultation, Technical Assistance, and Support: HHS assesses public health and medical effects resulting from all hazards. Such tasks may include the following:
Assessing exposures on the general population and on high- risk population groups
Conducting field investigations, including collection and analysis of relevant samples
Conducting field investigations, including collection and analysis of relevant samples
Providing technical assistance and consultation on medical treatment and decontamination of injured/contaminated individuals.
Behavioral Health Care:
Assessing mental health and substance abuse needs
Providing disaster mental health training materials for disaster workers
Providing liaison with assessment, training, and program development activities undertaken by Federal, State, Tribal, and jurisdictional mental health and substance abuse officials
Providing additional consultation, as needed.
Public Health and Medical Information: HHS provides public health, disease, and injury prevention information that can be transmitted to members of the general public.
Vector Control:
Assessing the threat of vector-borne diseases
Conducting field investigations, including the collection and laboratory analysis of relevant samples
Providing vector control equipment and supplies
Providing technical assistance and consultation on protective actions regarding vector-borne diseases
Providing technical assistance and consultation on medical treatment of victims of vector-borne diseases.
Potable Water/Wastewater and Solid Waste Disposal:
Assessing potable water, wastewater, solid waste disposal issues, and other environmental health issues
Conducting field investigations, including collection and laboratory analysis of relevant samples
Providing water purification and wastewater/solid waste disposal equipment and supplies
Providing technical assistance and consultation on potable water and wastewater/solid waste disposal issues.
Victim Identification/Mortuary Services:
Providing victim identification and mortuary services
Establishing temporary morgue facilities
Performing victim identification by fingerprint, forensic dental, and/or forensic pathology/anthropology methods
Processing, preparation, and disposition of remains.
Veterinary Services: HHS, in coordination with ESF #11, assists in delivering healthcare to injured or abandoned animals and performing veterinary preventive medicine activities, including conducting field investigations and providing technical assistance and consultation as required.
Medical Care Personnel is a key functional area of the ESF #8 response. The USPHS Commissioned Corps provides public health, humanitarian, and clinical services and personnel during an emergency, disaster, or other urgent public health need. Based on lessons learned from Hurricane Katrina, the USPHS adopted a tiered response posture of rapidly deployable, well-trained, and well-equipped teams. Below is a brief description of the USPHS teams currently available. Other USPHS teams may be phased in across coming years as the USPHS continues to examine and enhance its response capability.
Overview of USPHS Commissioned Corps teams
Rapid Deployment Force (RDF): The RDF consists of five pre-identified teams, each with 105 multidisciplinary staff. The teams serve on a rotating call basis, with the on-call team capable of deploying within 12 hours of notification. RDF teams have a built-in command structure and can provide mass care at shelters (including FMSs), staff Points of Distribution, and Casualty Collection Points. The RDF can also conduct community outreach and assessments, among other functions.
Applied Public Health Team (APHT): The APHT is composed of experts in applied public health and can function as a "public health department in a box." An APHT can deploy within 36 hours of notification and provide assistance in public health assessments, environmental health, infrastructure integrity, food safety, vector control, epidemiology, and surveillance.
Mental Health Team (MHT): The MHT consists of mental and behavioral health experts who assess stress and suicide risks within the affected population, manage responder stress, and provide therapy, counseling, and crisis intervention. The MHT can deploy within 36 hours of notification.
USPHS active duty officers who are not members of the aforementioned teams comprise supporting personnel who can deploy as teams or individuals within 72 hours of notification. Beyond the 72-hour mark, the USPHS Inactive Reserve Corps may be called on to augment the Active Duty Corps.
The National Disaster Medical System (NDMS) is another source of public health and medical personnel under ESF #8. The NDMS helps maintain our national capability to deliver quality medical care during domestic incidents that challenge or exceed normal medical capabilities or infrastructure in an affected area. NDM can provide assistance in three areas—field care, casualty evacuation, and definitive care—to support HHS under ESF #8 of the NRP.
Overview of NDMS teams
The NDMS is a nationwide partnership designed to deliver quality medical care to the victims of, and responders to, a domestic disaster. NDMS provides state-of-the-art medical care under any conditions at a disaster site, in transit from the impacted area, and into participating definitive care facilities. The main NDMS teams consist of the following:
Disaster Medical Assistance Team (DMAT): DMATs provide primary and acute care, triage of mass casualties, initial resuscitation and stabilization, advanced life support and preparation of sick or injured for evacuation. The basic deployment configuration of a DMAT consists of 35 persons; it includes physicians, nurses, medical technicians, and ancillary support personnel. They can be mobile within 6 hours of notification and are capable of arriving at a disaster site within 48 hours. They can sustain operations for 72 hours without external support. DMATs are responsible for establishing an initial (electronic) medical record for each patient, including assigning patient unique identifiers in order to facilitate tracking throughout the NDMS.
Disaster Mortuary Operational Response Team (DMORT): DMORTs work under the guidance of local authorities by providing technical assistance and personnel to recover, identify, and process deceased victims. Teams are composed of funeral directors, medical examiners, coroners, pathologists, forensic anthropologists, medical records technicians and transcribers, finger print specialists, forensic odontologists, dental assistants, x-ray technicians, and other personnel. HHS also maintains several Disaster Portable Morgue Units (DPMU) that can be used by DMORTs to establish a stand-alone morgue operation.
Veterinary Medical Assistance Team (VMAT): VMATs provide assistance in assessing the extent of disruption and need for veterinary services following major disasters or emergencies. These responsibilities include: Assessing the medical needs of animals, medical treatment and stabilization of animals, animal disease surveillance, zoonotic disease surveillance and public health assessments, technical assistance to assure food and water quality, and animal decontamination. Teams are composed of clinical veterinarians, veterinary pathologists, animal health technicians (veterinary technicians), microbiologist/virologists, epidemiologists, toxicologists and various scientific and support personnel. Deployment configurations depend on the nature and scope of the incident.
National Medical Response Team (NMRT): NMRTs provide medical care following a nuclear, biological, and/or chemical incident. This team is capable of providing mass casualty decontamination, medical triage, and primary and secondary medical care to stabilize victims for transportation to tertiary care facilities in a hazardous material environment. The basic deployment configuration of an NMRT consists of 50 personnel.
Additional medical care personnel are available through ESF #8 support agencies, such as the VA and DoD, and through the Medical Reserve Corps. During Hurricanes Katrina and Rita, the VA and DoD played significant roles in supporting ESF #8 missions. The VA (both facilities and personnel) was prominently involved in the operation of FMSs, while the DoD supplied aircraft, equipment, and personnel to facilitate the evacuation of patients and persons with special medical needs to facilities where they could receive appropriate care.
The Federal Government can also provide public health and medical equipment to support local response efforts during a public health emergency or disaster. One such deployable asset is the FMS, which can be used as a healthcare platform for stable patients with low acuity or primary healthcare needs. Below is a basic description of the FMS and its operating requirements.[81]
The Federal Medical Station (FMS) is an HHS deployable healthcare platform that can deliver large-scale primary healthcare services anywhere in the U.S. A team of approximately 100 personnel is needed to staff the FMS, with personnel provided primarily by the USPHS. Each FMS contains a three-day supply of medical and pharmaceutical resources to sustain 250 stable primary care based patients who require bedding services. Additional roles for the FMS may include the following:
Mass ambulatory vaccination services (using vaccination inventory from the SNS)
Ambulatory prophylactic medication administration (using medication inventory from the SNS)
Pre-hospital triage and initial stabilization for up to 250 mass casualty patients.
The FMS must be housed inside a structurally intact building that has roughly 40,000 square feet of space, a 10-person set up team, electricity, heating, air conditioning, ventilation, and clean water services. Reduced bed requirements can be accommodated in smaller facilities. Other operational requirements include bathroom and showering facilities, billeting for staff, and contracted support for food, potable water, laundry, ice, medical oxygen filling, and biomedical waste disposal. The FMS requires 48-96 hours from the time of request to delivery inside the continental U.S. and a 12-hour assembly time.
To address primary healthcare service needs far forward in a disaster area, HHS has a community outreach capability ("Go Bag") that is a rapidly deployable light strike team-based platform. Staffed primarily by the USPHS, each platform has basic medical and pharmaceutical resources to sustain 50 to 100 stable primary care based ambulatory patients.
7.4 HHS Concept of Operations for ESF #8
As the Primary Agency for ESF #8, HHS has developed a Concept of Operations Plan (CONOPS) that provides the framework for its management of the public health and medical response to an emergency or disaster. The HHS CONOPS is consistent with HSPD-5 and the NRP, and implements strategies to ensure a unified approach to all mitigation, preparedness, response, and recovery activities carried out by HHS. On behalf of the Secretary of HHS, the ASPR directs and coordinates all Federal public health and medical assistance provided under ESF #8. The ASPR also acts as the senior-level HHS liaison to DHS and other Federal departments and agencies.
Strategic coordination of the ESF #8 response
The ASPR coordinates the Federal ESF #8 response through the HHS Emergency Management Group or EMG, which operates from the SOC at HHS headquarters in Washington, D.C. By definition, the EMG is always operational at a baseline level and in times of non-response, it maintains a surveillance and monitoring posture. When preparing for or responding to an incident, the ASPR may raise the staffing level of the EMG and begin operations out of the SOC. The EMG's organizational structure is based on ICS principles.
The SOC is the focal point for command and control, communications, specialized technologies, and information collection, assessment, analysis, and dissemination for all HHS components under non-emergency and emergency conditions to support a common operating picture. It is continuously staffed and maintains operations 24 hours a day, 7 days a week (24/7). Because the SOC is always operational, it can rapidly enhance its services and staffing during times of crisis. When not in an emergency response mode, the SOC performs continuing surveillance of the following:
Public health data for special topics (e.g., West Nile virus, influenza activity)
Reports from Regional Emergency Coordinators (RECs), HHS OPDIVS and other ESF #8 agencies that support State, Tribal, and jurisdictional incident management
Media reports and other mass public information sources
Natural disasters (e.g., earthquake activity, hurricanes).
Watch Officers in the SOC maintain daily contact with other Federal operations centers to ensure situational awareness. Reports of incidents with potential public health or medical consequences are provided to the Duty Officer, who then alerts HHS senior staff as necessary. Critical public health and medical requirements are brought to the attention of the ASPR. During an event, the ASPR may deploy HHS liaisons to other Federal EOCs.
In addition to the SOC, some HHS OPDIVs, such as the CDC, maintain EOCs to manage their own assets. The OPDIV EOCs can be activated separately from the SOC when involved in a small-scale or "routine" response that does not require HHS department-wide coordination. However, when an OPDIV EOC is activated (only the SOC and the Director's EOC or DEOC at the CDC are operational 24/7), the EOC must notify the SOC and provide status updates of activities. During a department-wide response, the OPDIV EOCs coordinate their operational information with the SOC to establish a common operating picture. During response operations, staffing the SOC with experts from the HHS OPDIVs and Federal partners enhances ESF #8 coordination.
Operational coordination of the ESF #8 response
At the field level, the IRCT acts as the Secretary's agent on scene under the direction of the EMG. The IRCT consists of 10 pre-identified teams, with 30 multidisciplinary staff on each. The teams serve on a rotating call basis, with the on-call team capable of deploying within 12 hours of notification. The IRCT has a built-in command structure and is responsible for directing all ESF #8 response assets in the field. The IRCT is scalable to meet the demands of the incident. The IRCT coordinates the activities of all Federal ESF #8 resources deployed to assist States, Tribal Nations, jurisdictions, and other Federal agencies (see below). This includes teams deployed through HHS OPDIVs and the ESF #8 support agencies.
Key Roles of the IRCT
The IRCT is primarily responsible for supporting the public health and medical management of an incident. It does this by providing the field management component of the Federal public health and medical response. The IRCT is not designed to provide direct medical or mental-health care, decontamination, or public health services. Rather, the IRCT performs the following primary functions:
Provides liaisons in the field to coordinate with jurisdictional, Tribal, or State incident management
Provides the field management and coordination for deployed HHS and other ESF #8 assets to integrate those assets with the State and local response
Assesses the requirements or potential needs for HHS and ESF #8 assistance
Provides continuous assessment of the adequacy of the HHS and ESF #8 response to the Secretary through the ASPR
Represents ESF #8 in the JFO and the RRCC
Provides data management and information processing services for ESF #8. This includes the development of incident action plans and situational reports for the ESF #8 response
Acts as the conduit for incident information exchange between the SOC and the field (via the IRCT Leader).
Consistent with NIMS, each IRCT has a team leader and other appropriate personnel to fill ICS positions (Figure 7-1).[82] The IRCT Leader typically is an HHS Regional Emergency Coordinator (see description below); however, the ASPR maintains the right to appoint another qualified person to fill this position. To better coordinate all ESF #8 response components, the IRCT has liaisons from HHS OPDIVs and ESF #8 support agencies to integrate all ESF #8 activities under a single ICS. Any team from an OPDIV or ESF #8 support agency (e.g., VA, DoD) that is deployed during a disaster must report to that agency's liaison at the IRCT.
Figure 7-1. IRCT Organizational Chart
During large-scale or complex incidents, the Secretary of HHS may also deploy a Senior Health Official (SHO) to serve as his/her direct representative in the field. The SHO is typically an Admiral from the USPHS Commissioned Corps. When deployed, the SHO is responsible for overarching coordination of deployed HHS resources and provides guidance and leadership to the IRCT. The SHO essentially acts as an Agency Executive, as described in ICS, to the IRCT. The SHO serves in the JFO Coordination Group as the principal ESF #8 liaison to the PFO and other senior Federal, State, Tribal, and jurisdictional officials.
HHS has a cadre of regionally based personnel who work with State and local authorities on a variety of public health and medical initiatives, including preparedness and response to major events. It is important for public health and medical planners to understand the roles of these regionally-based personnel and to establish working relationships with them during preparedness planning to facilitate Federal support in a crisis. Brief descriptions of key regional personnel are provided below and their respective roles in preparedness, response, and recovery are summarized in Figure 7-2.
Regional Director (RD): An HHS political appointee at the regional level, the RD is the Secretary's regional representative and the primary spokesperson for HHS in his/her region, except in times of emergency. During normal daily operations, the RD reports pertinent information on regional issues and implications to HHS leadership. The RD promotes preparedness by coordinating regional resources through a Regional Advisory Council. During a response, the RD serves as the point of contact (POC) for elected officials and consults with an IRCT deployed to his/her region.
Regional Health Administrator (RHA): Oversees HHS public health programs at the regional level and coordinates with State Health Directors. The RHA builds relationships with State and local public health officials as well as other Federal departments in their region. During a response, the RHA may serve in a public health advisory role supporting the REC, and as a liaison to State Health Directors. The HHS Secretary may also call on the RHA to serve as the SHO, if needed.
Regional Emergency Coordinator (REC): Leads the HHS regional preparedness effort in his/her region by working with medical and public health planners to determine precisely what their response capability is, when they might need to ask for Federal support, and how they would integrate Federal assets into their ICS. The REC also is the HHS lead for regional response and typically serves as the IRCT Leader.
Regional Administrator (ACF): Serves as the liaison and advisor to the REC for coordination of Human Services (ESF #6) issues and participates in regional planning activities. During an event, the ACF RA assesses and coordinates the ACF response and provides a liaison to the IRCT.
Senior Management Official (CDC): Represents CDC in the State health department and coordinates technical support to local and State public health agencies. During a response, the SMO advises the State on the effective use of CDC assets and provides technical assistance and guidance.
Figure 7-2: Roles of HHS Regional Personnel in Emergency Management| Position | Preparedness
| Response
| Recovery
|
|---|
| RD: Sole political appointee in region | SUPPORT
Primary POC for elected officials
| SUPPORT
Primary POC for elected officials
| LEAD
Coordinates overall recovery efforts
Facilitates acquisition of necessary Federal resources
|
|---|
| RHA: Principal public health authority | SUPPORT Work with State Health Directors
Serves as a liaison for Assistant Secretary of Health to State health
| SUPPORT Serves in public health advisory role as requested and in support of the REC
Liaison with State Health Directors
May serve as SHO
| SUPPORT Facilitates recovery effort with State Health Directors
Maximize HHS investment in region
|
|---|
| REC: Leads HHS regional efforts in emergency preparedness and response | LEAD Regional lead for preparedness
Works will all State health officials and State emergency managers
| LEAD Lead for ESF #8 regional response
IRCT Team Leader
| SUPPORT POC for recovery but triages requests for support to the appropriate office
|
|---|
| ACF RA: Human Services coordination | SUPPORT Liaison and advisor to the REC
Participates in regional planning activities to plan for human service programs
ACF is responsible for HHS ESF#6 related activities
| SUPPORT Assesses and coordinates ACF response Provides a liaison to the IRCT
Provides support to program recipients
ACF is responsible for HHS ESF#6 related activities
| SUPPORT Coordinates human services support
Recommends program areas which may need support during recovery
ACF is responsible for HHS ESF#6 related activities
|
|---|
| SMO: Coordinates technical support from CDC to the States | SUPPORT Works in the State health department and represents CDC
| SUPPORT Advises States on the use of CDC assets and provides technical assistance
| SUPPORT
|
|---|
| SHO: HHS Secretary's direct representative in the field during an event | SUPPORT
| Deploys as needed at direction of Secretary Oversees IRCT field activities
Provides strategic level decision making and liaison between the PFO/FCO and HHS field activities
| SUPPORT |
|---|
The EMG deploys liaisons to field operations centers (e.g., JFO) to represent the Federal public health and medical response effort. Following the lessons learned from Hurricane Katrina, the JFO has been restructured along ICS lines, with ESF #8 liaisons within each ICS Section. The senior HHS liaison at the JFO is the SHO (if deployed).
The framework by which HHS responds to threats or public health emergencies is characterized by three general stages: notification and alert, deployment and operational management, and transition and disengagement. Each of these stages is described in detail below.
Notification and Alert
HHS learns about credible threats to the public's health, as well as potential or actual emergencies, from public health and emergency management authorities at all levels of government, disease surveillance systems, law enforcement agencies, intelligence channels, agricultural, industrial, and environmental agencies, and the media. The SOC is the notification point within HHS for public health threats and emergencies, and it should be contacted immediately (via established local to State to Federal communications channels) with any information regarding a threat or emergency.
Once notified, the SOC performs a series of pre-determined notifications within HHS, including the ASPR, the Secretary, the Deputy Secretary, and key members of the EMG staff. Depending on the nature of the incident, the ASPR may notify other senior Departmental officials, OPDIV EOCs or Heads, key Federal EOCs, and the relevant RHA, RD, and REC. As situational awareness is gained, the ASPR directs further actions, which may include activation of the EMG, which deploys liaisons to other Federal EOCs and/or places ESF #8 response teams or personnel on alert status.
The EMG also convenes an ESF #8 conference call to assess the situation and determine the appropriate actions. The EMG alerts pre-designated HHS personnel to represent ESF #8 on the following:
National Response Coordination Center (NRCC)
Regional Response Coordination Center (RRCC)
Emergency Response Team – National (ERT-N)
Emergency Response Team – Advance (ERT-A)
Joint Field Office/Joint Information Center.
Deployment and Operational Management
The Secretary of HHS, through the ASPR and the ESF #8 EMG, directs the activation and deployment of ESF #8 assets in support of State, Tribal, or jurisdictional incident management. The EMG activates an IRCT as required to coordinate locally the activities of all deployed ESF #8 assets and to represent ESF #8 in interactions with the affected local, State, or regional response structure. If there are multiple incidents, or one incident with widespread implications, the EMG may deploy multiple IRCTs. As stated earlier, the Secretary may also deploy a SHO to serve as the senior ESF #8 advisor in the JFO Coordination Group and to provide overarching field-level guidance and leadership to the IRCT.
At the request of the EMG, HHS OPDIVs and ESF #8 support agencies provide liaisons to the SOC to ensure a common operating picture and a coordinated ESF #8 response. Similarly, HHS may be asked to provide liaisons to other operations centers. The SOC schedules video and/or audio conferences at regular intervals to facilitate communications between the different components of the ESF #8 response and affected State, Tribal, and local authorities.
During incident operations, HHS oversees and coordinates appropriate missions under ESF #8 in accordance with FEMA mission assignments (if the Stafford Act has been invoked). EMG staff review each mission assignment received from FEMA to determine the most appropriate resource to meet the identified need. In some cases this may be an asset within HHS; in others, the EMG tasks its ESF #8 support agencies to provide the necessary resource(s). Through regular communications with the IRCT Leader, the EMG assesses the status of all ESF #8 mission assignments and anticipated future public health and medical needs.
Transition and Disengagement
The Secretary of HHS, through the ASPR, decides when to demobilize ESF #8 assets based on the successful completion of ESF #8 mission assignments and assessments of the overall public health and medical response. The demobilization of ESF #8 assets, including those from HHS OPDIVs and ESF #8 support agencies, is coordinated with the IRCT. With the demobilization of the IRCT, full responsibility for coordination with incident authorities transitions back to the regional staff and to any OPDIVs with regional assets stationed on a day-to-day basis in the region.
7.5 Integration with Other Tiers
Requests for Federal public health and medical support should specify the need for assistance, rather than ask for specific Federal assets. Thus, a key component of preparedness planning for emergency managers is determining the precise capabilities of the State, Tribal, and jurisdictional response systems, and establishing the process for recognizing when Federal public health and medical assistance may be indicated. Some basic considerations for preparedness planning are the following:
What are the full public health and medical response capabilities for the State or Tribe (including such resources as community health centers, long-term care facilities, Tribal Hospitals, VA Hospitals, and intrastate/interstate mutual aid arrangements)?
What types of hazard-generated demands can the response system handle? What demands may exceed the State or Tribe's resources (e.g., victims requiring isolation, casualties from an uncontrolled radiation release)?
What criteria will be used to determine when the State or Tribal response system is severely challenged (i.e., when the need for Federal support arises)? How will the decision-making process occur, especially early in an event?
What information or data will be necessary to define the specific requests for Federal assistance? How will this information be collected, collated, and analyzed at the State or Tribal level under the stress and time constraints of a large-scale or very unusual incident? Identifying the types of information that are important to convey when making a request for Federal assistance is an importance step of preparedness planning for State, Tribal, and jurisdictional emergency managers.
With a Stafford Act Declaration, the defined need for Federal assistance is transmitted via an Action Request Form (ARF) from the State EOC to the Operations Section within the DHS/FEMA JFO.[83] The ARF delineates who, what, where, when, and how much assistance is needed. Staff at the JFO reviews the eligibility of the ARF under the Stafford Act (i.e., is the need beyond the response capabilities of local, State, or Tribal authorities?) and, if it is eligible, converts the ARF into a mission assignment. The mission assignment is a work order by FEMA to a Federal agency that directs completion of a specific task. Depending on the need, FEMA will issue the mission assignment to the Primary Agency of the ESF with responsibility in that functional area. As the Primary Agency for ESF #8, HHS is issued mission assignments related to the provision of public health and medical assistance.[84] Once a mission assignment is issued, the EMG then determines, based on its internal resources and those of its OPDIVs and ESF #8 partners, the most appropriate way to accomplish the mission.
As Hurricane Katrina showed, the process for requesting and mobilizing Federal assistance can be time-consuming and cumbersome to meet urgent public health and medical needs in a disaster. HHS RECs have begun working with State public health and medical planners in their region to pre-identify areas where Federal public health and medical assistance will likely be necessary in an emergency or disaster. This may allow for the pre-scripting of common mission assignments so they can be issued quickly in a disaster. State public health and medical planners should work with their respective RECs to define areas where pre-scripted mission assignments may be warranted.
In the event that public health and medical assistance is activated under ESF #8, Federal resources will be tactically integrated into the appropriate State, Tribal, or jurisdictional ICS. This is essential because Federal assets are meant to support State, Tribal, and jurisdictional response efforts, not supplant them. To facilitate integration, Federal response teams should be briefed on how an emergency response is being managed at the State, Tribal, or jurisdictional level (where the primary incident management is occurring, who the lead management authority is, etc.).
On behalf of ESF #8, the IRCT receives tactical direction (e.g., instructions on where to report) from the appropriate State, Tribal, or jurisdictional authorities. Before Federal ESF #8 assets arrive on scene, a primary point of contact or liaison should be established. This may be the State's senior public health official or his/her designee. For State public health and medical planners, other critical preparedness planning considerations include the following:
Where will Federal support be staged and operate once it is committed to the State, Tribal, or jurisdictional incident response?[85]
What processes are in place to integrate external assets into State, Tribal, or jurisdictional incident management?
If the SNS is activated, is there an SNS plan in place that addresses:
How the SNS will be broken down once it arrives?
What priority system will be used to dispense SNS assets (e.g., elected officials, first responders, family members of first responders)?
How will the SNS be distributed to the public? If distribution centers have been established, how will the assets get there?
How will personnel responsible for distributing SNS get to the distribution centers? Have alternate plans been established?
If an FMS is activated, how will it be coordinated with the overall State and/or jurisdictional public health and medical response?
Have existing structures been identified to house FMSs?
Is there a protocol or mechanism available to provide operations support to the FMS?
How will patients be transported to an FMS and/or back to their primary area of residence?
Although Federal ESF #8 response teams will coordinate with State, Tribal, and jurisdictional incident management on tactical issues, the EMG, as directed by the ASPR, provides overall strategic direction to the IRCT Leader. The coordination of incident planning and response activities among Federal agencies occurs at the JFO.
7.6 Illustrative Example
The following example demonstrates how the concepts presented in this chapter may be applied during an actual incident response. The various phases of response (as described in Chapter 1) highlight when critical actions should occur; however, the example extends only as far as incident operations, as this is the focus of the MSCC Management System.
Background and Incident Description
A large, 7.0-magnitude earthquake occurs, with the epicenter near a metropolitan area on the New Madrid Fault in the central United States.
The earthquake occurs at dusk. Widespread loss of electrical power in the affected area limits the effectiveness of aerial flyovers for initial assessment. Early reports indicate that multiple cities and towns across the region are severely affected, with hundreds of structures reported to be collapsed, partially collapsed, or unusable.
Initial reports indicate that hundreds of people may be dead.
Given the severity of the event, the early response stages unfold fairly rapidly as follows:
Incident recognition at the Federal level occurs almost immediately, as the REC in the affected area rapidly contacts the SOC Watch Officer to report that a major earthquake has occurred. The SOC is also notified of the event from the DHS NOC. At the same time, the SOC Watch Officer receives initial media reports from national news agencies describing the incident. It becomes immediately obvious that Federal public health and medical assistance are indicated.
The SOC immediately notifies the ASPR, who alerts the Secretary of HHS. The ASPR activates the EMG, which establishes operations in the SOC, and notifies and briefs senior managers at HHS headquarters and at the OPDIVs.
Notification/activation of Federal public health and medical assistance occurs in anticipation of the Governor's request for a Presidential disaster declaration and implementation of the Stafford Act (in accordance with the Catastrophic Incident Annex of the NRP). An IRCT and RDF are placed on alert and prepare for deployment to the affected area. In addition, HHS convenes a call with ESF #8 support agencies to discuss the situation and possible assets that may be needed to provide public health and medical assistance.
Meanwhile, the REC establishes contact with local public health and medical officials, and the RD establishes contact with elected officials of the affected States, Tribal Nations, and jurisdictions. This initiates the process for potential Federal public health and medical assistance under ESF #8 once a disaster declaration is made and specific missions have been authorized. HHS also deploys personnel on the ERT-A to gain better situational awareness of potential public health and medical needs.
Mobilization at the national level is marked by an increase in staffing at the SOC, and by the deployment of HHS liaisons to staff other Federal operations centers, such as the DHS NOC and FEMA NRCC. In addition, the EMG deploys an IRCT and RDF to the disaster area. As the presumptive IRCT Leader, the REC begins the initial assessment of public health and medical needs and relays this information to the EMG. In addition, the Secretary of HHS appoints a SHO to serve in the JFO Coordination Group, once it is established.
RHA and regional ESF #8 staff coordinates with DHS through the EMG.
REC reports to the RRCC to begin coordinating requests for public health and medical assistance.
HHS OPDIVs and ESF #8 support agencies mobilize their EOCs, enhance staffing, and provide liaisons to the SOC to coordinate response activities.
In anticipation of requests for Federal public health and medical assistance, ESF #8 assets are forward deployed to mobilization centers on Federal property.
Incident operations activities are closely coordinated among jurisdictional, State, Tribal, and Federal officials. A JFO is established locally to bring together all key Federal, State, and jurisdictional stakeholders with incident management responsibility. Once on scene, the IRCT integrates into the JFO and the IRCT Leader coordinates all Federal ESF #8 resources that have been deployed. The IRCT Leader interacts with the State public health official(s) and emergency managers at the State EOC and relays information back to the SOC for accurate real-time situational awareness. The State EOC has activated its preplanned procedure for centralizing requests for public health and medical assistance from jurisdictional and State authorities and determines whether requests can be met using State resources or assets immediately available through mutual aid arrangements with neighboring States.
Once it is determined that Federal assistance for resources or assets is indicated, the State submits the request to the DHS request process through the JFO. Once the JFO has the request, DHS/FEMA distributes a mission assignment to the Primary Agency of the appropriate ESF. For public health and medical requests (ESF #8), HHS is tasked and has the responsibility to fulfill the mission assignment in coordination with its OPDIVs and ESF #8 support agencies.
The IRCT Leader provides situation reports to the EMG on a regular schedule, and all HHS response actions at the scene are coordinated with the EMG and other Federal operation centers (e.g., JFO, NOC-NRCC). Based on information contained in these situation reports, the ASPR, on behalf of the Secretary, coordinates the following ESF #8 functions:
Coordinates the deployment of immediate medical care (e.g., NDMS and USPHS Commissioned Corps) to help provide required public health and medical services in heavily affected communities
Coordinates the deployment of FMSs to serve low acuity patients and persons with special medical needs
Coordinates patient movement with DoD and the VA
Coordinates with the Medical Reserve Corps to support personnel requirements
Deploys healthcare personnel from the USPHS Commissioned Corps and NDMS to support hospitals that are short-staffed
Engages with HRSA to assist in evaluating affected Community Health Centers
Deploys experts from FDA to provide consultation regarding safe feeding of displaced populations
Tasks CDC to provide technical assistance on injury prevention and public health missions
Tasks CDC to assist in monitoring the health of emergency workers, and to provide technical assistance on worker health and safety measures and precautions
Tasks CMS to assist in monitoring and enforcing or waiving/suspending HCF regulations
Tasks SAMHSA to assist in providing mental health crisis counseling
Tasks IHS and other relevant Federal agencies to assess potable water and waste-water/solid waste disposal issues resulting from loss of power and water utilities.
The HHS Assistant Secretary of Public Affairs collaborates with the DHS Public Affairs Office on all public affairs aspects of the response. Public affairs response teams are deployed to address media inquiries, to develop public information materials, and to provide public information liaison officers to the IRCT and to other Federal operations centers. The primary Joint Information Center (JIC), established in support of the NRP, provides general health and medical information to the public after consultation with HHS.
70.In the context of this document, jurisdiction refers to a geographic area's local government, which usually has the primary role in emergency response. A definition of local government is provided in Appendix D.
71. The NRP definition of a catastrophic event is provided in Appendix D.
72. ESF #8 support agencies are identified in the ESF #8 annex of the NRP.
73. HHS OPDIVs include the Centers for Disease Control and Prevention (CDC); Centers for Medicare and Medicaid Services (CMS); Food and Drug Administration (FDA); Indian Health Service (IHS); Health Resources and Services Administration (HRSA); Substance Abuse and Mental Health Services Administration (SAMHSA); National Institutes of Health (NIH); Agency for Healthcare Research and Quality (AHRQ); Administration for Children and Families (ACF); and Administration on Aging (AoA).
74. The definition of an Incident of National Significance is provided in Appendix D.
75. The NRP was originally published in December 2004; it was updated in May 2006 based on organizational changes in DHS and lessons learned from Hurricanes Katrina, Rita, and Wilma. At the time of this writing, the NRP is undergoing further revisions. Incident operations activities are closely coordinated among jurisdictional, State, Tribal, and Federal officials. A JFO is established locally to bring together all key Federal, State, and jurisdictional stakeholders with incident management responsibility. Once on scene, the IRCT integrates into the JFO and the IRCT Leader coordinates all Federal ESF #8 resources that have been deployed. The IRCT Leader interacts with the State public health official(s) and emergency managers at the State EOC and relays information back to the SOC for accurate real-time situational awareness. The State EOC has activated its preplanned procedure for centralizing requests for public health and medical assistance from jurisdictional and State authorities and determines whether requests can be met using State resources or assets immediately available through mutual aid arrangements with neighboring States.on. Readers are encouraged to visit the DHS Web site periodically for the latest updates to the NRP.
76. Definitions of these multiagency structures are taken from: Department of Homeland Security, "Notice of Change to the National Response Plan," May 25, 2006. Readers are encouraged to access the NRP on the DHS Web site for more information.
77. The NRCC is one of five sub-elements of the NOC; the other sub-elements include Interagency Watch, Information and Analysis Component; National Infrastructure Coordination Center; and Operational Planning Element.
78. Appendix B describes ICS and its application to public health and medical disciplines.
79. The DHS/FEMA-led ERT-A is the principal interagency group that conducts assessments and initiates coordination with the State and initial deployment of Federal resources.
80. Members of the Task Force include AdvaMed, American Association of Blood Banks, American Association of Tissue Banks, American Hospital Association, American Red Cross, America's Blood Centers, Armed Services Blood Program Office, Blood Centers of America, CDC, College of American Pathologists, FDA, Plasma Protein Therapeutics Association.
81. Readers are encouraged to work with their regional emergency coordinators to learn more about the FMS and state/local responsibilities for its operations.
82. In the event of multiple incidents, or one incident with widespread implications (e.g., Hurricane Katrina), multiple IRCTs may be mobilized at the discretion of the ASPR.
83. Prior to the establishment of a JFO, requests for Federal assistance should be made to the RRCC.
84. Not all ESF #8 mission assignments are issued directly to HHS; for example, DoD is tasked directly by FEMA to support the evacuation of patients and persons with medical special needs from a disaster area. Though it is directly tasked, DoD coordinates all activities related to this mission assignment with HHS.
85. Federal assets deployed in anticipation of need are commonly "staged" on Federal property, such as military bases, prior to being assigned to State, Tribal, or jurisdictional management.